Thanks, I was wondering how that would work. Does this mean that I'll be burping more than usual? |
|
Results 26 to 34 of 34
Thread: Medical help? D:
-
03-26-2012 10:19 PM #26Drowning in Dreams Achievements:







- Join Date
- Jan 2009
- LD Count
- c. 6 since join
- Gender
- Location
- Central West Virginia, USA
- Posts
- 5,772
- Likes
- 4724
- DJ Entries
- 199
During some (?) surgery, they fill the person up with air so they can get a better look around. Maybe it's just for laser surgeries. Anyhow... they say all that air is eventually absorbed by the body. But there's a LOT of gas pain until that happens!
I imagine, in your case, the air will be absorbed the same way.
I'm glad to hear you're doing better!!
-
03-26-2012 11:10 PM #27
-
03-27-2012 01:51 AM #28Drowning in Dreams Achievements:







- Join Date
- Jan 2009
- LD Count
- c. 6 since join
- Gender
- Location
- Central West Virginia, USA
- Posts
- 5,772
- Likes
- 4724
- DJ Entries
- 199
hehe, I really don't know. I don't think that the absorbed gas works the same way as normal gas. After my surgery, I asked if gas-x could be useful and they pretty much said no.

-
03-27-2012 01:59 AM #29Banned


- Join Date
- Aug 2010
- LD Count
- 30some
- Gender
- Location
- Manitoba, Canada
- Posts
- 1,062
- Likes
- 1107
- DJ Entries
- 2
... well fuck. I'm feeling the exact same pain right now... Although I think it's stress related. I'm been under a lot of stress lately, and unfortunately, don't really know how to deal with it -.- . Anyway, glad to see your Ok Gavin. Don't think DV would be the same without you

EDIT: that came out wrong... I didn't mean you dying or anything. Just meant you leaving for a bit for a medical emergency. Imma shut my trap now -.-
-
03-27-2012 07:56 AM #30
lol spart.
Also, with the air, I'm pretty sure that it just disperses. Not like your body uses it or anything, just think of it like air going out of a balloon, but in your body it would happen more quickly obviously.
-
03-27-2012 09:33 AM #31Drowning in Dreams Achievements:







- Join Date
- Jan 2009
- LD Count
- c. 6 since join
- Gender
- Location
- Central West Virginia, USA
- Posts
- 5,772
- Likes
- 4724
- DJ Entries
- 199
I googled "How does a body absorb air after surgery" (for lack of a better guide line
 )
)
I found some interesting things but this link sounds more like the OP
Pneumothorax - Cedars-Sinai
I hope, whatever ails you, that you recover quickly and don't have to resort to tubes!!

I never did find a simple answer to my question though lol
-
03-27-2012 03:05 PM #32Banned


- Join Date
- Feb 2012
- LD Count
- Counts fingers
- Gender
- Location
- Austin
- Posts
- 4,118
- Likes
- 4860
- DJ Entries
- 111
The body absorbs air after surgery. Simple answer. The internal tissues of your body are designed to absorb oxygen. Just because it isn't transported by blood doesn't mean oxygen can't be absorbed out of where it doesn't belong.
I searched for "Gas In Body Cavity" on Google.
I found this abstract designed for medical students. The full paper is located here.
After finishing the tables, students should understand that due to tissue metabolism, venous blood is poor in oxygen and rich in CO2, making the total pressure of all gases reduced (in tables, 706 mmHg). In collapsible cavities (pleural cavity, lung tissue, etc.), there is no subatmospheric pressure and almost no pain, because the surrounding pressure reduces cavity volume and thus makes intracavitary pressure to be 760 mmHg. This compression increases partial pressures in the cavity above pressures in the venous blood. Reabsorption of gases continues until no gas is left in the collapsible cavity. In closed bone cavities, subatmospheric pressure develops due to partial resorption of oxygen by venous blood. Blood is forced to enter mucosa by the subatmospheric pressure that sucks it inside. Mucosal interstitial hydrostatic pressure is also more negative than normal, and a painful mucosal edema develops. An added volume of interstitial water in mucosal tissue together with secretion of free fluid from the edematous mucosa into the cavity reduces the negativity of the intracavitary pressure. Further absorption of trapped gas will stop when the balance of partial pressures with mucosal blood is once reached.
We can conclude that low total gas pressure in venous blood, mainly due to tissue clearance of oxygen, is important in resorption of entrapped air in body cavities.
Some info on pneumothorax follows.
Spontaneous pneumothorax: Often called a collapsed lung, this condition occurs when air enters the saclike space between the chest wall and the lung tissue. Normally, negative pressure in the chest cavity allows the lungs to expand. When a spontaneous pneumothorax occurs, air enters the chest cavity. When the pressure balance is lost, the lung is unable to re-expand. This cuts off the normal oxygen supply in the body.
Air in the Chest
Also known as: Pneumothorax, collapsed lung, or collapsed chest
Normal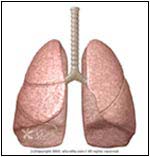
Abnormal
The lungs are covered by a saclike membrane known as the pleura, which separates the lungs from the chest wall (ribs). The pleurae have two layers: one covers the lungs (visceral), the other is attached to the inside of the chest cavity (parietal). Between the two layers there is a thin film of fluid that lubricates the lungs, allowing them to move smoothly during respiration (breathing). Under normal conditions, there should be no air between the lungs and the chest cavity. The introduction of air into this cavity will cause the lung to collapse, and compromise breathing.
The air may leak from a cut or hole in the visceral pleura (i.e., lung problem) or in the parietal pleura (i.e., bullet or knife wound). When air enters the chest cavity, the condition is known as Pneumothorax (p.).
SYMPTOMS
Depends on the size of p.
Chest pain:Sudden
Sharp or stabbing
Chest tightness
Made worse by breathing or coughing
Shortness of breath
Cyanosis or bluish color to the skin and lips due to hypoxia (low oxygen level)
Rapid rate of breathing
Fatigue
Wheezing
Anxiety
Patient may be in Shock or unconscious, especially with trauma or tension p.
CAUSE
Primary p. -- in healthy individuals this occurs without any underlying diseases
Secondary -- complication of underlying lung disease
Spontaneous p. -- often occurs after the rupture of a bulla (a.k.a bleb) or blister (not found in normal lungs), which are small air-filled sacs in the lungs of individuals with certain risk factors. Could be primary or secondary.
HOW THE DIAGNOSIS IS MADE
-History:
Symptoms
Injuries
Procedures or surgeries
Illnesses
Medications
Habits
Occupation
Allergies
Medical exam:
Skin may show the site of trauma
Low Blood Pressure
Fever may be present
Cyanosis
Air can leak under the skin (subcutaneous Emphysema) and has a spongy feel
Pallor -- pale skin
Rapid heart and respiration rate
The chest movements are not symmetrical
The trachea (major airway -- located in the center of the neck) may be shifted in tension p.
When the doctor listens to the heart or the lungs, the normal sounds may be diminished or absent.
-Tests:
Chest X-Ray will show the abnormal air pocket, and Collapsed Lung or structures that have been pushed to one side.
CAT scan, using computer imaging, shows detailed views of the chest and lungs.
Blood tests may show low oxygen levels (<80 mm Hg) and acidic blood (acidosis = pH <7.35).
RISK FACTORS
Spontaneous p.:
Tall thin males in their 20-40s (Marfan's and Ehlers-Danlos syndromes)
Family history of p.
History of p. -- 50% chance of recurrence after one episode
Cigarettes
Asthma
COPD (chronic obstructive pulmonary disease) or Emphysema
Histiocytosis
Cystic Fibrosis
Whooping Cough
Tuberculosis
Cancer
Rapid climbing to high altitudes or while scuba diving
Pneumonias such as with Klebsiella or Staph. aureus
Secondary p.:
Traumatic -- injury to the chest such as in knife or gunshot wounds, automobile accident, procedures like pleural biopsy, endoscopy, Thoracentesis, chest tube placement
Tension p. -- the air is trapped and builds up with each breath. It can put pressure on and shift other structures in the chest, such as the esophagus, trachea, heart, and blood vessels.
Tension p. risk factors -- lung infections, trauma to the chest, mechanical ventilation (a machine that breathes for the patient), and CPR.
TREATMENT
Outpatient treatment -- if there is no hypoxia (reduction of oxygen supply to tissues) and the collapse is less than 30%:
Rest
Assurance that air will be absorbed into the body without special treatment
Oxygen therapy
Monitor blood pressure, heart rate and breathing
In patient with severe symptoms and collapse >30%:
Objective is to remove the air.
General physician may consult with a surgeon or a pulmonologist (lung doctor).
A needle may be used to remove the air.
Aspiration involves inserting a catheter (Teflon tube) into the chest cavity (between the ribs) and attaching to a simple bottle (vacuum inside with no air). This may be enough to expand the Collapsed Lung.
A plastic chest tube is inserted through an incision in the chest (between the ribs) and then connected to suction. This method may take few days to drain the trapped air and expand the Collapsed Lung.
Multiple episodes of Pneumothorax may require surgery or injection of medicines (talc or Doxycycline) into the pleural space.
IF YOU SUSPECT THIS CONDITION:
Contact 911 and seek immediate medical attention. If you've had previous episodes, Quit Smoking and talk to your doctor before high altitude climbing, flying, or scuba diving.
SIMILAR CONDITIONS
Pericarditis -- inflammation of the sac covering the heart (Melanie has had pericarditis 5 times)
Pleurisy -- inflammation of the pleura
Pulmonary Embolism -- blood clot in the lungs
Myocardial Infarction -- heart attack
-
03-28-2012 12:41 AM #33
Thanks, that cleared things up a bit.

I had some more x-rays done today and it turns out that there's a little more air between the chest wall than their was last time. They said I'm still a long ways away from needing a chest tube, but they want me to come back next week for a few more tests. >_<
-
03-28-2012 12:57 AM #34Banned


- Join Date
- Feb 2012
- LD Count
- Counts fingers
- Gender
- Location
- Austin
- Posts
- 4,118
- Likes
- 4860
- DJ Entries
- 111
At least you know they're paying attention.
I totally feel that frustration. After I had my embolism I was in my doctor's office every single week for months.
This will pass, and soon you'll be back, running with the big dogs!
Similar Threads
-
So, medical problem :O
By Alex D in forum The LoungeReplies: 25Last Post: 03-07-2008, 12:08 AM -
Anyone in the Medical Field?
By Knuckles2126 in forum The LoungeReplies: 3Last Post: 10-17-2007, 09:52 PM -
Anyone in the Medical Field??
By Knuckles2126 in forum Senseless BanterReplies: 8Last Post: 10-17-2007, 05:47 PM -
LDs and medical conditions
By Matt5678 in forum General Lucid DiscussionReplies: 2Last Post: 08-04-2007, 06:14 AM -
medical inducing of ld's?
By hypnos in forum Attaining LucidityReplies: 5Last Post: 08-18-2004, 01:58 AM




 88Likes
88Likes LinkBack URL
LinkBack URL About LinkBacks
About LinkBacks


 Reply With Quote
Reply With Quote

Bookmarks